Major new audit launched to improve lymphoma care in Northern Ireland
Northern Ireland
A major new programme to better understand and improve care for people with blood cancer in Northern Ireland has been launched by Lymphoma & Leukaemia Northern Ireland (LLNI) and Blood Cancer UK, working in partnership with the Northern Ireland Cancer Registry (NICR) at Queen’s University Belfast.

Leuakaemia & Lymphoma Northern Ireland, Blood Cancer UK and the Northern Ireland Cancer Registry
The programme will, for the first time in over 15 years, bring together a comprehensive epidemiological report covering blood cancers including leukaemia, lymphoma and myeloma, alongside a detailed clinical audit focused on lymphoma care.
Together, this will provide the clearest picture yet of how people with blood cancer are diagnosed, treated and supported across Northern Ireland.
Current figures suggest that more than 8,700* people are living with, or in remission from, blood cancer in Northern Ireland, with over 850 people diagnosed each year.
This insight will help us identify where care is working well and where we can improve services for our patients in the future.”
- Dr Oonagh Sheehy, Consultant Haematologist
Blood cancer in Northern Ireland
Blood cancer is the fifth most common cancer in the region and the third biggest cancer killer, claiming more than 330 lives annually including over 130 deaths from lymphoma and around 110 from leukaemia each year.
Despite advances in treatment, there has been no comprehensive regional audit of blood cancer care since 2008, meaning gaps remain in understanding how care varies across the system and where improvements are needed.
By combining real-world clinical data from treatment centres with population-level registry data, the programme will identify variation in care, highlight examples of best practice, and support services to deliver more consistent, evidence-based treatment.
Dr Oonagh Sheehy, Consultant Haematologist, at Belfast Health & Social Care Trust, said:
“Blood cancer is a group of cancers which includes leukaemia, lymphoma and myeloma. Each of these diseases has distinct ways of presenting and can respond differently to therapy. Lymphoma is highly complex with over 50 known subtypes, which can make it difficult to measure and track outcomes.
“By linking detailed clinical information from hospitals with registry data, we’ll be able to build a much clearer understanding of how patients with lymphoma are diagnosed and treated across Northern Ireland. This insight will help us identify where care is working well and where we can improve services for our patients in the future.”
The work will build on the last comprehensive audit of lymphoma care carried out by NICR in 2008. Since then, treatment approaches, diagnostics and clinical pathways have evolved significantly.
The Northern Ireland Cancer Registry (NICR) at Queen’s University Belfast, led by Director Dr Damien Bennett, will provide a backbone of high quality, comprehensive, population-level data and Dr Stephen Quinn and Sinéad Hawkins (Audit Analysts) at NICR, will analyse patients diagnosed more recently allowing comparisons with quality indicators used in other UK nations and helping clinicians understand where Northern Ireland is performing well and where improvements could be made.
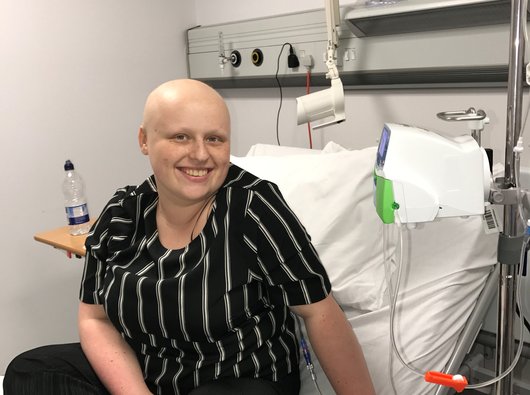
For patients, like Jacqueline Stewart, it has the potential to make a real difference. Jacqueline from Belfast, was first diagnosed with lymphoma at 18, and said:
The audit is already underway, with clinicians across Northern Ireland contributing data. To date, the Northern Ireland Cancer Registry has received almost 100 patient records from healthcare professionals.
An epidemiological report is expected to be published in summer 2026, with the wider audit findings due later in the year.
The potential to make a real difference
Jacqueline's story
For patients, like Jacqueline Stewart, it has the potential to make a real difference. Jacqueline from Belfast, was first diagnosed with lymphoma at 18, and said:
“Being diagnosed with lymphoma at 18 completely blindsided me. At that age, you just never think it’s going to be you. My whole life changed overnight, and in many ways my twenties have revolved around cancer including treatment, hospital appointments, and recovery. It felt like everything was put on pause.
“I’ve been through multiple rounds of chemotherapy and a stem cell transplant, and there were times it was incredibly tough both physically and mentally. You spend a lot of time on your own, and there’s always that worry in the back of your mind that never fully goes away.
“But I also know how fortunate I’ve been to receive such good care. From the moment I was diagnosed, I felt like I was in safe hands, and that made such a difference during the hardest times. I’m now back at work and getting my life back, and that means everything. Projects like this are so important because they can help make sure everyone gets the same standard of care and support. If it helps even one person have a better experience or get through treatment more easily, it’s worth it.”
Stephanie McMullan, Business & Operations Manager from Leukaemia & Lymphoma NI said:
“This audit will be the first of its kind since 2008 and the first blood cancer report in Northern Ireland to include information related to multiple myeloma. In addition, the clinical audit will focus on Lymphoma, with additional data being provided by patients and clinicians. This will allow us to better understand the quality and consistency of care for patients across Northern Ireland and make comparisons with other parts of the UK. We believe the insights from both parts of this audit will translate into meaningful improvements for patients and families in NI.”
Helen Rowntree, Chief Executive at Blood Cancer UK, said:
“Blood cancers are the third biggest cancer killer in the UK, yet historically they haven’t always received the same level of focus as other cancers when it comes to understanding care pathways and outcomes. Projects like this are incredibly important because good data drives better care. By working with partners in Northern Ireland, we can start to build a clearer picture of how lymphoma patients are diagnosed and treated, where services are working well, and where more support is needed. Ultimately, that knowledge will help ensure people affected by lymphoma receive the best possible care, wherever they live.”
"Projects like this are so important because they can help make sure everyone gets the same standard of care and support. If it helps even one person have a better experience or get through treatment more easily, it’s worth it.”

