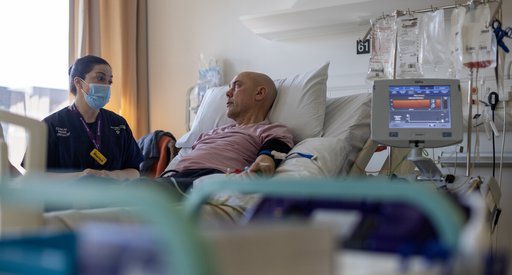
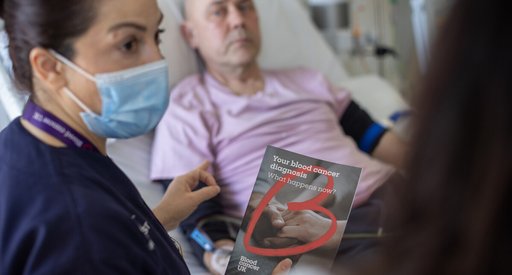
Healthcare Professionals
You might also be interested in

Our research projects
Discover all the current research we are funding into different types of blood cancer.
Latest news
Stay updated with the latest blood cancer news including information about new treatments and research projects we are funding.

Our campaigns
We campaign to reach the day where no lives are lost to blood cancer, and we need your support.