This MDS World Awareness Day, four people share their story
Every year over 2,000 people in the UK are diagnosed with a type of blood cancer called myelodysplastic syndromes (MDS). But many people have never heard of it. On 25 October, World MDS Awareness Day aims to fix that.
This year a group of people living with or in remission from MDS helped us create a new information booklet about this type of blood cancer. Here, four of them share their story.

Ally was diagnosed with MDS in 2008
Giving up the job I loved was devastating
When Ally first started feeling nauseous and fatigued in April 2007, he put it down to stress and exhaustion. He had a busy job in the fire service, his wife was pregnant and they were moving house, so it was a stressful time.
Over the next few months, Ally was feeling more and more unwell and unable to work. He was tested for lots of viruses, but no one suggested anything serious was going on. So when Ally eventually got the diagnosis of MDS, it came as a total shock.
One of my first questions when I was diagnosed was ‘Can I go back to work?’ The haematologist said I had bigger things to worry about. But to me, that was my biggest worry.
After his diagnosis, Ally worked in the fire service for another six years. But in 2014 he had to admit he wasn’t well enough to do the job anymore, so medically retired. He talked to us about how he found a new purpose in life, raising awareness of stem cell donation and patient involvement.
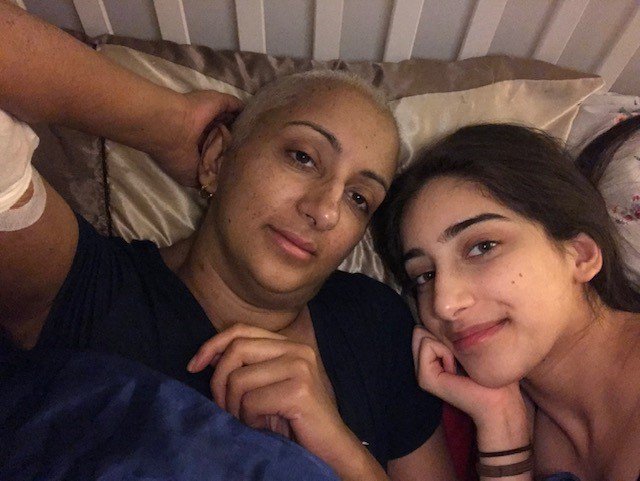
Kal, pictured on the left with her daughter, was diagnosed with MDS in 2019
My brother's stem cells saved my life
Like many people with MDS, the first symptom Kal noticed was feeling really tired. She put it down to a busy lifestyle, but then her periods became really heavy to the point they just weren’t stopping. Extreme tiredness, getting lots of infections and bleeding more than usual can all be symptoms of MDS.
After a referral to a haematologist and a bone marrow biopsy, Kal got the news she had MDS. Her doctor told her she was at high risk of it turning into another form of blood cancer called acute myeloid leukaemia (AML). The risk of this happening varies from person to person, but overall it affects between two and three out of every 10 people with MDS.
Kal’s best chance of stopping this happening, and potentially curing the MDS, was to have a stem cell transplant. But as an Asian woman, she knew her chances of finding an unrelated donor were much lower than for people from white backgrounds.
Luckily, Kal’s brother was a match, and she had a successful stem cell transplant. We spoke to her about her experience.

The road to beating MDS
Professor Ghulam Mufti explains how things have changed for people with MDS throughout his career, the exciting progress made in genetics, and how we'll go about curing MDS on a global scale.

Emma was diagnosed with MDS in 2011
My tips for long hospital stays
Emma was diagnosed with MDS in 2011. Over the years, Emma has needed lots of treatment including blood transfusions, immunosuppressive therapy, chemotherapy and two stem cell transplants. All this has meant spending a lot of time in hospital.
Emma’s built up a packing list of things she takes into hospital to keep active, fight boredom and feel more like herself.
I’d take so much stuff into hospital with me, I think the nurses thought I was absolutely bonkers, bringing a yoga mat with me while having chemotherapy!
We spoke to Emma about her hospital essentials and the advice she’d give to others.

Peter was diagnosed with MDS in 2017
Continuing to work with side effects
The way MDS develops and the treatment needed vary a lot from person to person. Many people can continue to work while having treatment for MDS.
When Peter was diagnosed with MDS, he admitted early on to his employer that he was struggling with the diagnosis. He asked what support was available and his employer was able to offer him counselling. It set him up with a good foundation to understand his feelings around the diagnosis, and how to create coping mechanisms.
Peter shared his story of working with MDS, and the things that helped him.

Order your free guide to MDS
Ally, Emma, Kal, Peter and other people with MDS share their advice and tips in our free guide to diagnosis, treatment and living well with MDS.
